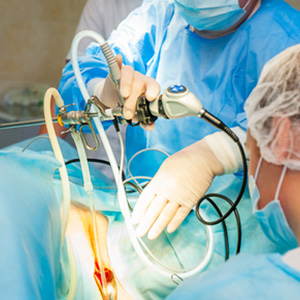
Laparoscopy
Laparoscopy is a procedure where a laparoscope, a probe with a telescopic end, is inserted into a small incision in the abdomen, enabling the viewing of the pelvic and abdominal regions. In this procedure, a small amount of carbon dioxide gas is injected into the region to separate the organs and make them easier to view. In most cases, laparoscopy has a faster recovery time and is less time-consuming and expensive than more invasive surgical procedures such as laparotomy.
Laparoscopy is the best way to assess the abdominal/pelvic organs, because they can be seen as they really are, compared to a manual pelvic examination or viewing of images by x-ray or ultrasound.
Initially, laparoscopy was used only as a diagnostic procedure enabling the physician to visually inspect the inside of the pelvis (diagnostic laparoscopy). That was once possible only through opening of the abdomen, a major surgery. Over a period of time, with improved skills of laparoscopists and better instrumentation, operative interventions became possible (operative laparoscopy). Most types of pelvic surgery have been attempted by laparoscopy.
Operative Laparoscopy
Operative laparoscopy has gained tremendous acceptance and publicity for one reason: recovery after the procedure is much easier and shorter. Physicians are still discussing why this is the case.
Some of the suggested reasons include:
- A smaller incision is made in the abdomen (2 or 3 1/2 inch cuts or less) compared to 3 or 4 inches in open surgery (laparotomy).
- Use of carbon dioxide seems to be tolerated better than exposure of the inside of the abdomen to the room air.
- Better visualization of individual pelvic organs, frequently compared to the surgeon having an "eye on the end of the scope."
There may other reasons which are not well understood and are still being discussed.
The field of operative laparoscopy is ever-increasing. At its beginning approximately 30 years ago, the cutting of adhesions, aspirations of cysts, or burning of intra-abdominal lesions, most frequently Endometriosis, was considered to be a risky procedure. Now laparoscopy has evolved to a state where removal of the uterus, kidney, ovaries, etc. are common procedures. Removal of the appendix and gall bladder, together with laparoscopically-assisted vaginal hysterectomy, are typical procedures which show a significantly lesser recuperation time and less pain.
ome time ago, laparoscopy was a special privilege for gynecological surgeons, who had to prove their skills, training and abilities prior to being allowed to perform these more involved abdominal procedures. Nowadays, training in laparoscopy, diagnostic as well as operative, is part of every residency training program.
Second-Look Laparoscopy
There are situations where a re-visitation of the pelvis is called for. This became much easier with the invention of laparoscopy.
The two major reasons for second-look laparoscopy are if the surgical procedure is better performed in two steps, or if the surgical procedure exposes the patient to the risk of significant formation of adhesions. An adhesion is a scar which forms after a procedure. Various patients have different tendencies to form scarring, and these tendencies are practically impossible to predict. For that reason, if the surgeon suspects a high likelihood of significant formation of adhesions, second-look laparoscopy is called for. If timed properly, removal of forming adhesions should be easy, and cause essentially no complications.
Hysteroscopy
This procedure involves the insertion of a thin, lighted, telescope-like instrument known as a hysteroscope through the vagina and cervix into the uterus. This enables the full examination of the uterine cavity. Hysteroscopy for diagnostic purposes can be done in the doctor's office with local anesthesia and mild to moderate sedation, or in an operating room with full anesthesia when significant intrauterine changes are suspected. Most pathological changes within the uterus can be dealt with at the time of hysteroscopy under anesthesia.
Most frequent hysteroscopy findings are intrauterine adhesions (synechia), polyps or tumors within the uterine cavity, and closure of the tubes at the uterine opening (ostia). All these conditions can be handled satisfactorily by an experienced hysteroscopist using appropriate equipment. The adhesions, polyps and tumors can be re-sected with special instrumentation and the proximal closure of the fallopian tubes opened. These operations are somewhat tricky, but in the hands of an experienced surgeon complications should be rare.
Myomectomy
In some cases, benign uterine tumors - leiomyomas, called myomas or fibroids - may be a reason for infertility or repeated pregnancy loss, but not always. There is no general agreement among infertility specialists about the significance of myoma. Each patient's history and situation must be considered individually.
The size of the tumors and their location need to be carefully investigated by all available means.
If removal of the tumors (myomectomy) is necessary, the procedure can be done by laparoscopy, hysteroscopy or open surgery- laparotomy. There are two main goals for performing this operation:
- Removal of all tumors and repair of the uterine wall to allow pregnancy and preferably vaginal delivery.
- Avoidance of postoperative adhesions/scarring.
Various surgical techniques and postoperative regiments were designed to accomplish both goals.
Myomectomy is known to frequently produce significant postoperative adhesions. For this reason, the patient may end up without tumors, but with a large amount of adhesions, and therefore still be unable to conceive. The options should be discussed by the patient and her doctor, but the decision about the method should be left to the doctor, who has the patient's confidence and sufficient experience with this type of surgery.
Repair of Previous Tubal Sterilization
Since the discovery of the function of the uterine tubes, it became obvious that a closure of this conduit would prevent unwanted pregnancies. Various surgical techniques were developed to accomplish that. Care should be taken to sacrifice the portion of tube keeping in mind that the patient may require re-canalization in future.
After tubal sterilization, in some situations family circumstances change and repair of tubal closure and recanallization of at least one of the tubes becomes desired.
Results of surgery to reopen the tubes depend on how much of the tube was removed - that is, how much of the tube remains and is usable - as well as on the surgical skills of the operating surgeon. Significant improvements in results have been noticed since the early 70's, when an operating microscope started to be used in the reconstruction of the tube. Introduction of the microscope demanded the development of special microsurgical instruments and techniques.
Hydrosalpinx Hydrosalpinx - It is a Disease Hydrosalpinx (a fallopian tube closed at the end and distended with fluid) has been known to the medical profession for ages. It is usually a consequence of pelvic infectious/inflammatory disease spreading into the fallopian tubes and pelvis via the cervix and uterus. Some of these diseases manifest themselves with significant clinical symptoms (pain, fever, malaise, nausea). However, some of them might go unnoticed because the symptoms of pelvic infection/inflammation are mild and may be misinterpreted as urinary bladder infection or "bowel" problems.
For patients who have hydrosalpinx on both sides of the fallopian tube, the only possible chance for having a "natural" conception is surgery. Because of the delicacy and intricacy of tubal surgery, new microsurgical techniques were developed by surgeons interested and experienced in this particular area.
The Society of Reproductive Surgeons was formed many years ago. Besides the repairing of fallopian tubes, the Society also became interested in other efforts of surgical correction of diseases which may affect the ability to conceive and cause numerous other health problems. Since the invention of IVF, surgery on fallopian tubes has been pushed off the main interest of infertility specialists, but not forgotten. Unfortunately, there are some centers were the only expertise available to infertility patients is IVF. Surgical experience and know-how might not be available.
Within the last year, a number of centers have reported the harmful effect of hydrosalpinx and a lower conception rate in patients who are undergoing attempts of IVF without repairing the tubal disease. Frankly, it is not surprising. There is no question that hydrosalpinx is a disease and disease is never good for any type of living organism, including the patient (carrier of the disease) and her embryos. In scientific reports, terms like "highly toxic fluid of hydrosalpinx" or "significantly toxic fluid" are routinely used to describe what happens to small embryos transferred into the uterine cavity that contains traces of fluid from hydrosalpinx leaking from the tube into the uterus. What is missing is information on the effect of this toxic substance on the well-being of the mother herself.
Microsurgery on fallopian tubes is making a comeback. Various centers recommend removal of the tube or closure of the connection from the hydrosalpinx into the uterus. However, a surgical repair of the hydrosalpinx remains the best way to deal with the diseased pelvic organs and their toxic effect on the mother and her baby.
Removal of the tube (salpingectomy) has been viewed with skepticism because once the tube is removed, there is no way to undo this particular procedure. A number of researchers have studied changes in ovarian function in situations where extensive destructive surgery is performed on the tube (or sometimes even lesser intervention, i.e., tubal sterilization). The tube and ovary share a significant part of the blood supply and destruction of one conceivably can affect the other.
Closure of the part connecting the hydrosalpinx with the uterus is not advisable. Normally, fluid from the fallopian tube leaks inside the uterine cavity, and thus does not cause excessive distention. Once this channel is blocked, the fluid has nowhere to go and the tube balloons up. Clinical experience has taught us that patients whose tubes are closed at both ends usually have extremely large hydrosalpinx, which sooner or later necessitates surgical intervention.
Surgical repair of the hydrosalpinx (salpingostomy) has been performed for decades. The success of the surgery was improved by careful pre-operative and post-operative management and the introduction of the surgical microscope and microsurgical techniques and instruments such as laparoscopy. This usually means a significant prolonging of the operating time itself, and not all physicians are willing to spend several hours in the operating room doing their best to re-establish the patency of the fallopian tubes. Thus, the domain of this type of surgery has been limited to a few reproductive surgeons. With the proper use of the available surgical techniques and pre and post-operative management, the results of reparative surgeries have been improving continuously.
It has been our firm belief that disease should be treated and wherever possible, eliminated. In today's systems of delivery of medical care, patients might hear more and more frequently that this or that disease, including hydrosalpinx, does not need to be treated. It does!
Based on experience and recent scientific data, we believe that hydrosalpinx should be treated even in patients who are not planning to get pregnant and definitely in those who are hoping to conceive.
Booking a visit
© 2017 Pushpaa Hospital

